Personal Viral Induced Wheeze Action Plan
What is Viral Wheeze
A wheeze or whistling sound that is caused by a viral infection (a cough or a cold). The wheeze may return each time your child has a cold. Usually the child is well in-between the viral infections but the wheeze can last for some weeks after the infection. Children under the age of 3-5 years are more likely to be affected as their air passages are small.
Treatment over the next few days
Over the next few days, your child will be recovering and hopefully will feel better.
They may still need their blue reliever inhaler (salbutamol) if they have symptoms of chest tightness, a dry cough or shortness of breath.
If they have symptoms, you can give up to 6 puffs of their blue reliever inhaler and the effects should last for 4 hours.
If your child becomes increasingly breathless or the effects are not lasting 4 hours, you should follow the instructions outlined in the RED section.
In the event that your child has been started on steroid tablets, these should be continued once daily (usual treatment course is 3 – 5 days for prednisolone or 1 day for dexamethasone).
You should continue your child’s normal preventer treatment(s) during an acute exacerbation of asthma.
If your child’s wheeze worsens in future, please follow the instructions outlined in red/amber/green traffic table.
If you / your child is:
- Too breathless to talk / eat or drink
- Has blue lips
- Having symptoms of cough/wheeze or breathlessness which are getting worse or not improving despite 6 puffs blue (salbutamol) inhaler every 4 hours
- Confused and drowsy
Ring 999 for immediate help.
Give 10 puffs of blue (salbutamol) reliever inhaler every 10 minutes until ambulance arrives.
Keep child in upright position and reassure them.
If you / your child is
- Wheezing and breathless
- Having a cough or wheeze/tight chest during the day and night
- Too breathless to run / play / do normal activities
Immediately contact your GP or 111 out of hours and make an appointment for your child to be seen that day face to face.
Increase blue (salbutamol) reliever inhaler up to 6 puffs and this should last 4 hours.
If using 6 puffs every 4 hourly and symptoms are not improving or getting worse, move to RED
If your child’s breathing is not laboured or fast and he/she is able to continue their normal day to day activities
Give 2-4 puffs blue (salbutamol) reliever inhaler every 4 hours until symptoms improve. If needing this more than 24hrs contact your GP or 111 out of hours
If you require more puffs move to AMBER
Choose appropriate sized spacer with mask (or mouthpiece if child is over 3 years with good technique and is not significantly short of breath)
- Shake the inhaler well and remove cap
- Fit the inhaler into the opening at the end of the spacer
- Place mask over the child’s face ensuring a good seal
- Press the inhaler once and allow the child to take 5 slow tidal breaths between each dose
- Remove the inhaler and shake between every puff
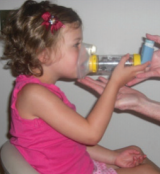

Repeat steps 2 – 5 for subsequent doses
Plastic spacers should be washed before 1st use and every month as per manufacturer’s guidelines
For videos on using your child’s inhaler and spacer correctly see goo.gl/235DQf 
No, not necessarily. This is a different condition from asthma, although a few children do go on to develop asthma. Asthma is rarely diagnosed before the age of 5 as the majority of children will grow out of viral induced wheeze.
If your child has multiple episodes of viral induced wheeze especially if they have factors that make them more likely to develop asthma, they are sometimes treated with similar medication to prevent episodes.
Children with asthma (who are not well controlled):
- Are often wheezy, even when they do not have a cough or cold
- Usually have a family history of asthma and allergy
- Are generally more breathless than their friends when they run around or become wheezy on exercise.
- Often have a regular night time cough
If you are worried that your child has asthma, you should make an appointment to see your GP or GP asthma nurse.
You should arrange for them to be reviewed by your GP if they continue to have lots of problems with wheeze once they have recovered from their cold.
- Make sure your child is not exposed to tobacco smoke. Passive smoking can seriously damage your child’s health. It makes breathing problems like viral induced wheeze worse.
- Remember smoke remains on your clothes even if you smoke outside.
If you would like help to give up smoking you can find information below:
Smoking and e-cigarettes :: Frimley HealthierTogether (frimley-healthiertogether.nhs.uk)



